Clinical Editors: Megan Dodson, PA-C & Alexander Kazberouk, MD
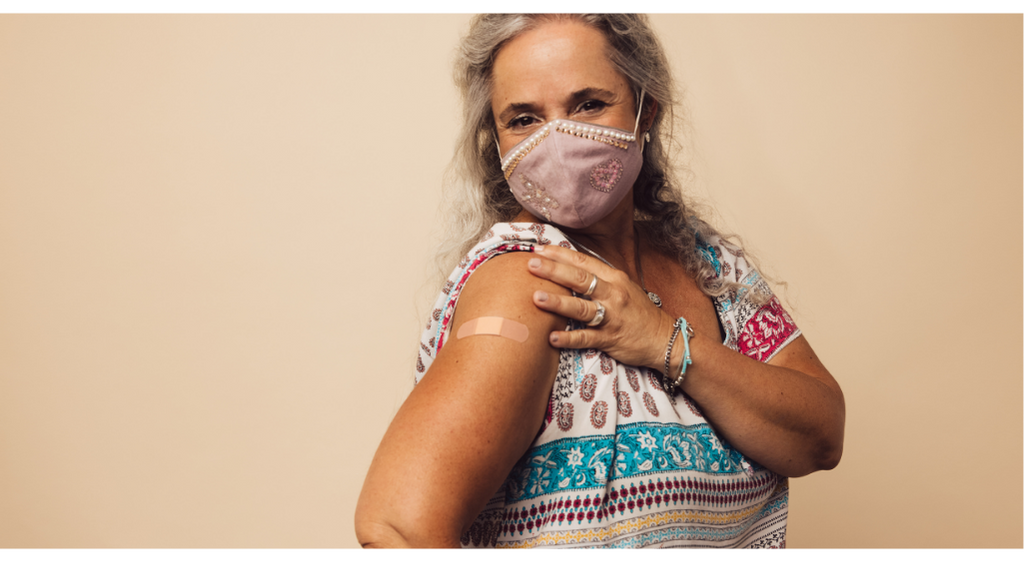
As we age, our immune system weakens over time, putting us at higher risk for contracting certain diseases and becoming sicker from those diseases as a result. There are several diseases that are higher risk for seniors, including shingles, the flu, and more recently, COVID-19.
According to the CDC, almost 1 out of every 3 people in the United States will develop shingles in their lifetime, and that risk increases as you age. For the 2019-2020 flu season, over 50 percent of seasonal flu-related hospitalizations occurred in people 65 years and older, with adults 65+ accounting for 72% of flu-related deaths. In 2023, COVID-19 related hospitalizations and deaths have also disproportionately affected the 65+ community, with seniors making up almost 90% of COVID-19 related deaths. Finally, Respiratory Syncytial Virus (RSV) leads to 6,000 to 10,000 deaths for older adults annually.
These numbers could be drastically reduced through vaccination and prevention. Here are answers to a few common questions we receive from seniors and their family members about which vaccines for seniors are necessary.
What vaccines do seniors need?
1. COVID-19
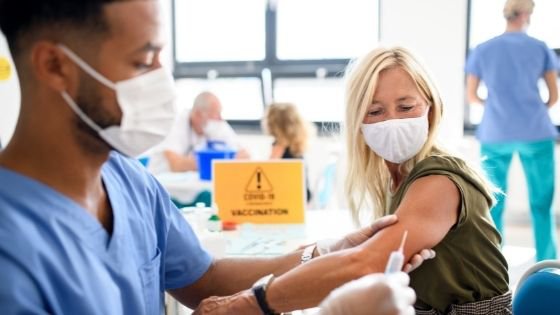
The COVID-19 global pandemic gave rise to the need to develop vaccines to combat the outbreak of a novel coronavirus (known as SARS CoV-2), the virus that causes the disease COVID-19. Coronaviruses are a group of viruses that can be spread primarily through droplets of saliva or discharge from the nose when an infected person coughs or sneezes. Symptoms range from mild to severe, with a number of cases becoming fatal.
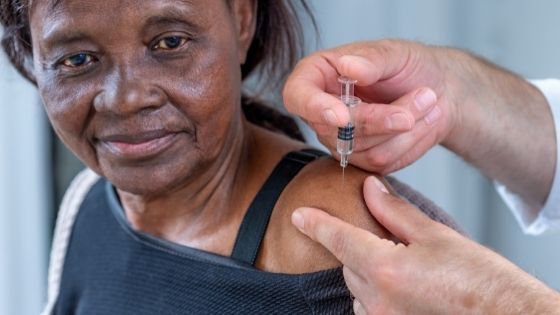
Older adults, and those with underlying medical problems like cardiovascular disease, diabetes, chronic respiratory disease, and cancer are more likely to develop serious illness. The Centers for Disease Control and Prevention (CDC) recommends that seniors 65+ receive two doses, four months apart, of the 3 updated COVID-19 vaccines available:
- Pfizer-BioNTech
- Moderna
- Novavax
The CDC does not recommend one COVID-19 vaccine for seniors over another– the best vaccine is the one that is available to you. If you have questions about any of the vaccines, reach out to your primary care provider.
2. Influenza (flu)
The flu is a viral infection that is treatable, but can be deadly to vulnerable groups like seniors or adults living with chronic health conditions such as asthma and diabetes. One of the best ways to protect yourself from the flu is to get an annual flu vaccination. According to the CDC, seniors 65+ should avoid the nasal spray influenza vaccine and should get any approved flu vaccine:
High dose flu vaccine
- Brand name: Fluzone High-Dose
- Contains four times more antigen (the part of the vaccine that helps your body build up protection against flu viruses) than the regular vaccine. This vaccine contains more antigen so older people have a better immune response, and therefore, better protection against the flu.
- Brand name: Flublok
- Contains three times more antigen than the regular vaccine and is approved for anyone 18 or older
Adjuvanted flu vaccine
- Brand name: FLUAD
- This is a standard dose made up of three inactivated flu vaccines with an adjuvant.
- An adjuvant is added to a vaccine to create a stronger immune response to vaccination.
The CDC does not recommend one flu vaccine for seniors over the other. If you have questions about which vaccine is right for you, reach out to your primary care provider.
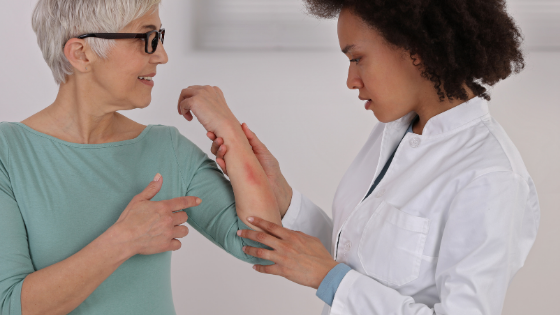
3. Shingles
Shingles is a painful rash that appears on the body and is considered a reactivation of the chickenpox virus. Before the rash appears, people may feel intense burning and numbness where the rash usually develops. Others may experience symptoms such as a fever, headache and fatigue.
Shingles typically lasts between two and six weeks though prescription antiviral medications are available to speed up the healing process. For seniors, complications from shingles can lead to serious, long-term health problems. The complications from shingles range from bacterial skin infections that can cause scarring to hearing and vision loss, nerve damage in the hands and feet and postherpetic neuralgia (PHN).
Because shingles is more likely to reactivate in older adults, a vaccine, Shingrix, is available and is highly recommended for adults ages 50 and older to prevent outbreaks. The vaccine is given in two doses, two to six months apart. Even if a person has had shingles in the past, they can still take this vaccine to prevent a future outbreak.
4. Tetanus
Tetanus is an infection caused by a bacteria, Clostridium tetani , which can be found in the soil. The bacteria can enter the body through open wounds or cuts in the skin. Tetanus symptoms can include painful spasms, muscle stiffness, difficulty swallowing, and even difficulty breathing. Symptoms May appear anytime from a few days to several weeks after the bacteria has entered the body.
Not only is tetanus more severe in seniors, but its complications are also more serious with risks. Seniors who get tetanus are more susceptible to broken bones from muscle spasms, difficulty breathing (respiratory failure), and other complications
According to a study done by the University of Tsukuba, Japan, tetanus is far more common in older adults, but can be prevented with vaccination. Adults should receive a preventive vaccine dose every 10 years, ensuring it is up-to-date if they ever get a cut in their skin, are bitten by an animal, etc. Adult vaccines for tetanus include:
- Tdap vaccine protects adults from tetanus, diptheria and whooping cough.
- Td vaccine protects adults from tetanus.
5. Whooping Cough

Whooping cough is a contagious respiratory tract infection. Once infected, it takes about seven to 10 days for the first signs and symptoms to appear. The symptoms may appear cold-like at first with symptoms that include:
- Runny nose
- Nasal Congestion
- Red, watery eyes
- Fever
- Cough
These symptoms worsen after about two weeks. Mucus accumulates inside the airways, causing an uncomfortable, “whoop”-sounding cough. Although many people do not develop the “whoop” characteristic, the coughing fits can be uncontrollable and painful.
Whooping cough can make babies and young children very sick, and so it is a great idea for seniors to make sure they are up-to-date with the vaccine if they have a grandchild that they wouldn’t want to get sick. Additionally, seniors are still susceptible to whooping cough, especially if the vaccination has worn off Even after recovery the cough can last for weeks! Some complications seniors may experience or develop include sleep apnea, insomnia, weight loss, pneumonia and eye infections.
Luckily, the whooping cough vaccination is safe and protects from other infections as well. Adults who have never been vaccinated for pertussis should get one dose.
6. Pneumonia
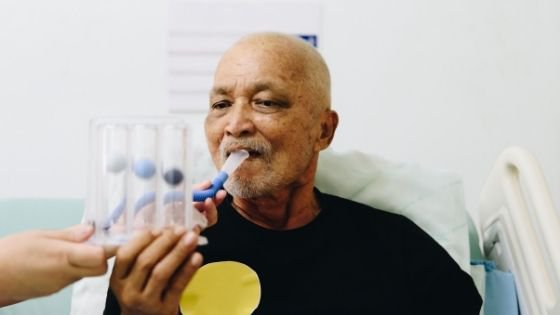
Pneumonia is an infection of the lungs that causes air sacs that may fill with fluid. According to the CDC, seniors 65 and older are more likely to get pneumonia. With symptoms ranging from mild to severe, it is important to make the distinction between pneumonia and milder upper respiratory infections.
There are quite a few symptoms of pneumonia which include:
- Chest pain when breathing or coughing
- Fatigue
- Fever, sweating and chills or low body temperature
- Nausea, vomiting or diarrhea
In seniors, a symptom of pneumonia may be confusion or changes in mental awareness. In terms of complications, pneumonia in the elderly can lead to several potentially severe health complications. These include:
- Bacteremia: A bacterial infection that can invade the body’s organs
- Pleurisy and Empyema: Inflammation of the lining of the lungs and infection of inflammatory fluids.
- Lung Abscess: A pus-filled cavity in the infected lung area
- Acute Respiratory Distress Syndrome (ARDS): When the lungs become severely injured from pneumonia, respiratory failure may occur.
The pneumonia vaccine is an essential for seniors, especially if they have never received a pneumococcal conjugate vaccine before. There are different kinds of pneumonia shots for seniors, and the CDC recommends one of the following pneumococcal vaccines for all adults 65 years or older:
- PCV20 (Pneumococcal conjugate vaccine): Protects against 20 strains of pneumococcal bacteria.
- PCV15 (Pneumococcal conjugate vaccine): Protects against 15 strains of pneumococcal bacteria.*
*If PSC15 is administered, the CDC recommends following the vaccine with a dose of PPSV23 (Pneumococcal polysaccharide vaccine), which protects against 23 strains of pneumococcal bacteria.
7. Respiratory Syncytial Virus (RSV)

RSV is an upper respiratory virus that generally causes milder symptoms such as sore throat, cough, fever, congestion, and fatigue. However, older adults are at an increased risk for complications such as pneumonia. Every year, 60,000 to 180,000 older adults are hospitalized for RSV in the United States and 6,000 to 10,000 die from it. RSV is especially dangerous for older adults with lung disease, heart disease, or those who are immunocompromised. In addition, RSV can cause very severe disease in young infants (especially those <6 month old or born premature).
RSV season is generally fall through early spring.
In 2022, two vaccines to prevent RSV were approved by the FDA:
These vaccines are very effective at preventing severe infections - a one-time dose is recommended for:
- Anyone 75 or older
- People 60-74 years old who are immunocompromised, have significant heart or lung disease, live in a nursing home, or have other risk factors that put them at risk for serious RSV infection
There are separate recommendations for pregnant people and younger children.
What are some common side effects of these vaccines?
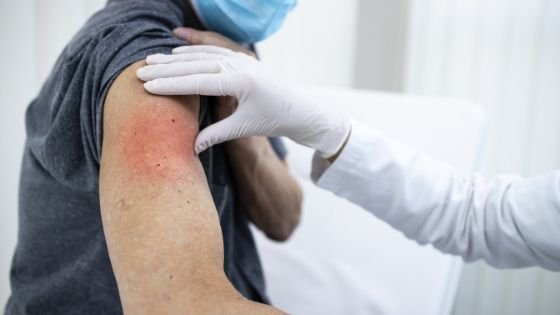
For most of the above vaccines, you might experience redness/swelling from the shot, headache, chills, nausea, muscle aches and tiredness.
Vaccine appointments and costs
For those on Medicare, where you get your vaccine matters. Some coverage plans may require you to receive your Shingles, Tdap or RSV vaccines at a pharmacy vs. in your doctor’s office. Talk to your insurance company or your provider about which vaccines are covered by insurance in your clinic or in the pharmacy.
These vaccines address the most common, preventable diseases that affect older adults annually. Your doctor can advise on any other vaccines that may be needed. At your next appointment, be sure to ask your doctor which vaccines are right for you.
With flu season right around the corner, make sure you’re up on these flu FAQs so you can be prepared.
Originally published August 14, 2021
The One Medical blog is published by One Medical, a national, modern primary care practice pairing 24/7 virtual care services with inviting and convenient in-person care at over 100 locations across the U.S. One Medical is on a mission to transform health care for all through a human-centered, technology-powered approach to caring for people at every stage of life.
Any general advice posted on our blog, website, or app is for informational purposes only and is not intended to replace or substitute for any medical or other advice. 1Life Healthcare, Inc. and the One Medical entities make no representations or warranties and expressly disclaim any and all liability concerning any treatment, action by, or effect on any person following the general information offered or provided within or through the blog, website, or app. If you have specific concerns or a situation arises in which you require medical advice, you should consult with an appropriately trained and qualified medical services provider.