Updated February 29, 2024
Clinical Editors: Megan Dodson, PA-C, Rocky Patel, MD, and Toni Ferrara, MSN, NP-C
When it comes to your heart health, you likely know how lifestyle factors like exercise and nutrition can impact your risk of disease. But how can you tell if you’re tracking in the right direction?
While a number of risk factors like personal and family health history can’t be measured, there are a few metrics that can help provide a picture of your heart health and fitness. Familiarizing yourself with these numbers can help you better understand your disease risk and manage your overall health. You can work with your primary care provider to set goals, make lifestyle changes, and reduce your risk of disease over time. Here are 3 metrics that relate to your heart health:
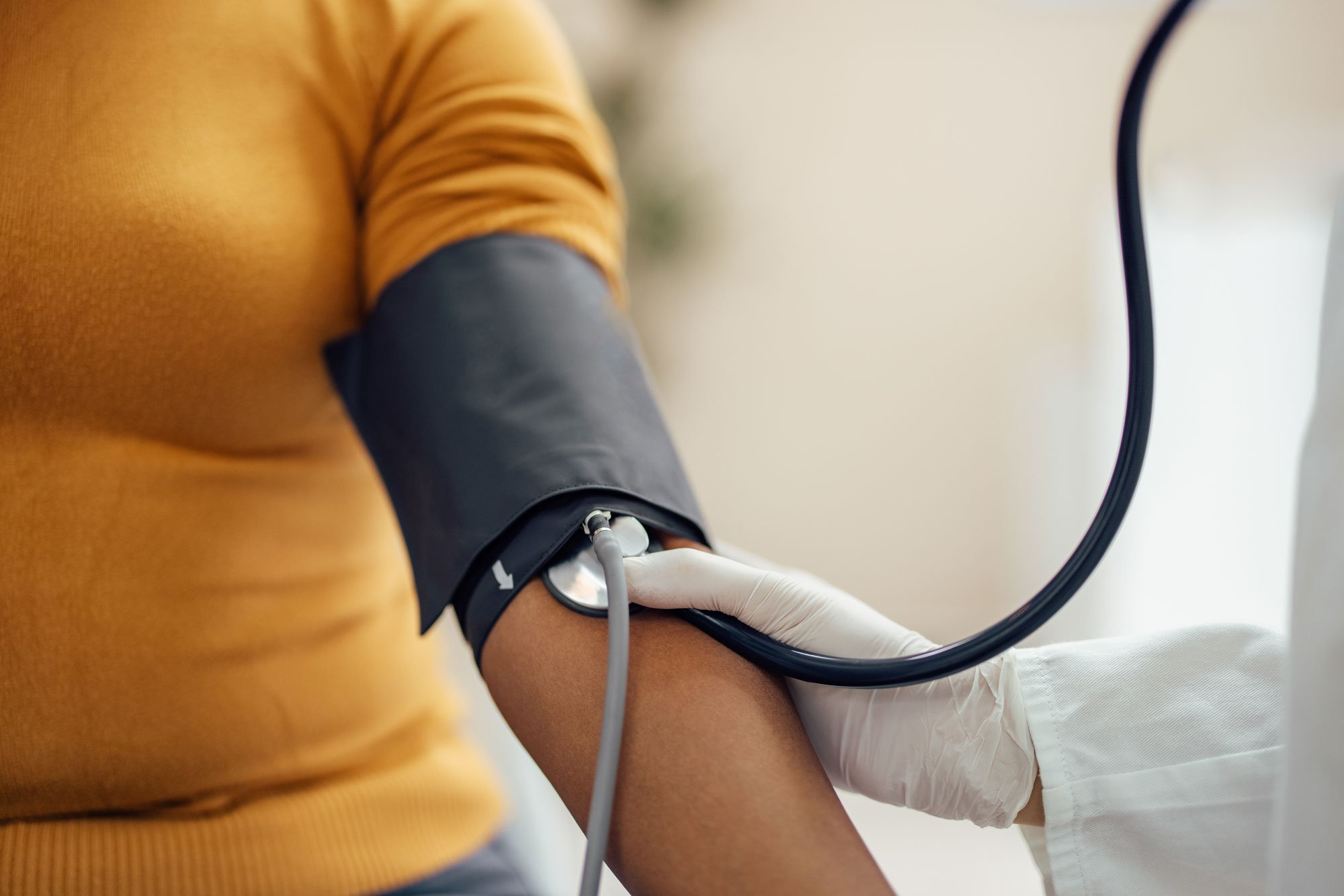
1. Blood pressure
Blood pressure refers to the force of your blood against the walls of your blood vessels. Each time your heart beats, it pumps blood through the arteries to the rest of your body. Your blood pressure is highest when your heart contracts, and lowest when it’s at rest. As a result, your blood pressure fluctuates slightly throughout the day as you exercise, eat, sleep, drink, and experience varying levels of stress. It can also change with age, medications, temperature, and number of other factors.
Blood pressure is measured in two numbers: The top number (systolic blood pressure), refers to the pressure in your arteries when you heart is beating, while the bottom number (diastolic) refers to the pressure when your heart is at rest. Anything less than 120/80 mmHg (millimeters of mercury) is considered to be within a healthy range. Elevated blood pressure is when the systolic number is between 120 and 129, and the diastolic number is still less than 80. High blood pressure (hypertension) is when the systolic number is at or above 130, or the diastolic number is between at or above 80.
Hypertension occurs when the force of your blood against the walls of your blood vessels is consistently too high. Over time, high blood pressure can cause significant damage to your blood vessels and other parts of your circulatory system, increasing your risk of heart disease, stroke, heart failure, and other chronic conditions.
As high blood pressure doesn’t typically cause any obvious symptoms, many people aren’t even aware they have it. That’s why it’s extremely important to regularly have your blood pressure checked so you can better understand your risk of disease and take preventive action.
Your primary care provider will check your blood pressure during your annual physical, and as needed in following appointments, depending on your risk factors and health history. If you have high blood pressure, they might even recommend using an at-home arm cuff to check your blood pressure over time. Learn more about measuring your blood pressure here.
2. Blood glucose
Blood glucose refers to the amount of glucose (a type of sugar) that is found in your blood. Your body creates blood sugar by digesting the food you eat into glucose – which is then transported through the bloodstream to be used for energy and stored in your cells for later use. Your pancreas produces an important hormone called insulin that helps your cells absorb and store glucose.
When this process goes smoothly, your blood glucose level fluctuates throughout the day and as you eat, insulin helps move glucose from the bloodstream to the cells. If you haven’t eaten for at least eight hours, a fasting blood glucose level of less than 100 milligrams per deciliter of blood (mg/dL) is generally considered healthy. Otherwise, a non-fasting blood glucose of less than 140 milligrams per deciliter (mg/dL) is also a good goal.
Too much glucose in your bloodstream over an extended period of time, however, can cause damage to the blood vessels, nerves, kidneys, and eyes, and can be a sign of diabetes — a condition that further increases your risk of heart disease.
Fortunately, monitoring your blood glucose level can help you prevent and reduce your risk of developing diabetes. Your provider may recommend checking your fasting blood sugar level, your non-fasting blood sugar level, or a test called hemoglobin A1c, which can also give information about your blood sugar without requiring fasting. Talk to your provider about whether blood glucose screening is right for you.
3. Cholesterol
Cholesterol is a type of fat that plays an important role in many bodily functions. It helps your body build cells, create vitamins, and produce hormones, as well as digest food. While cholesterol is necessary for a number of reasons, too much can raise your risk of heart disease and stroke.
A blood test called a “cholesterol panel” measures a few different types of cholesterol that can impact your heart health. While you may have heard of “good” or “bad” cholesterol, these terms aren't quite accurate. We actually need both types of cholesterol, but higher levels of LDL (also called “low density lipoprotein”) have been connected to an increased risk of heart disease. While it's important to know your individual cholesterol levels, It's best to work with your provider to understand how these numbers impact your overall heart disease risk.
As high cholesterol doesn’t typically have any symptoms or warning signs, the only way to know your cholesterol level is to get it checked through a blood test. Adults who are not taking cholesterol medication should have their cholesterol checked every four to six years. Depending on your personal health history, however, your primary care provider might recommend having your cholesterol checked more often. Learn more about ways to improve your cholesterol here.
What else you should know
Paying close attention to your blood sugar, blood pressure, and cholesterol levels can help you better understand your risk of heart disease and take control of your cardiac health. Your primary care provider can partner with you to create a personal care plan to keep your heart healthy, and help keep your numbers at a goal that’s right for you .
It’s important to note though, a number of other factors can also contribute to your heart health. Beyond these three metrics, lifestyle factors such as your alcohol consumption and tobacco usage, as well as your age, sex, waist circumference, medication usage, and personal and family medical health history can all contribute to risk of heart disease.
Regular visits to your primary care provider can help you understand your personal risk and stay on top of routine testing and screening. Your provider will treat you within the context of your overall health, to suggest lifestyle changes and ensure those changes are being optimized to best protect your long-term heart health.
Have more questions about these heart metrics or your general heart health? Our primary care team is here to help. At One Medical, we aim to provide exceptional care designed around you and your unique health needs. Sign up today to book a same or next day appointment — in person or over video — through our app.
The One Medical blog is published by One Medical, a national, modern primary care practice pairing 24/7 virtual care services with inviting and convenient in-person care at over 100 locations across the U.S. One Medical is on a mission to transform health care for all through a human-centered, technology-powered approach to caring for people at every stage of life.
Any general advice posted on our blog, website, or app is for informational purposes only and is not intended to replace or substitute for any medical or other advice. 1Life Healthcare, Inc. and the One Medical entities make no representations or warranties and expressly disclaim any and all liability concerning any treatment, action by, or effect on any person following the general information offered or provided within or through the blog, website, or app. If you have specific concerns or a situation arises in which you require medical advice, you should consult with an appropriately trained and qualified medical services provider.